Factors Associated With Dietary Behaviour Among Patients With Type 2 Diabetes Mellitus in Rural Indonesia
DOI:
https://doi.org/10.15605/jafes.037.02.02Keywords:
dietary behaviours, social support, type 2 diabetesAbstract
Background. Type 2 Diabetes Mellitus (T2DM) is one of the fastest-growing diseases and most serious major health problems worldwide. Few studies have focused on the association of social support with diabetes-related dietary behaviour.
Objective. To examine the relationship between social support and dietary behaviour among patients with diabetes in a rural area of Indonesia.
Methodology. This was a descriptive cross-sectional study that included 120 physically healthy patients above 18 years old with type 2 diabetes mellitus for at least 6 months. Data analysis was done using a stepwise regression model.
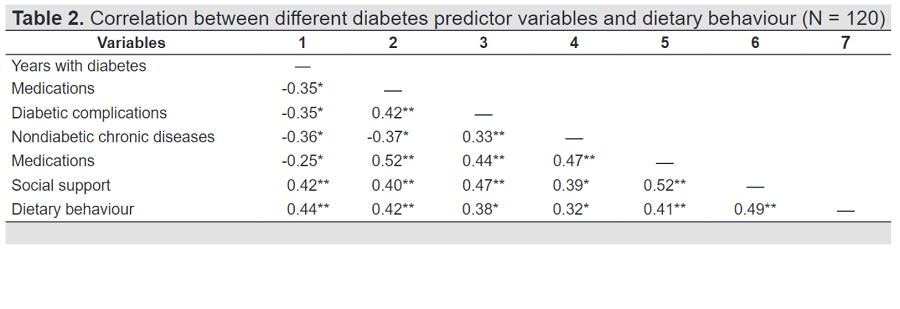
Results. The mean age was 61.97 years (SD = 7.85, range = 52-74); 86.7% of the participants were females. Social support (β = 0.272, p = <0.001), diabetes medications (β = 0.169, p = 0.003), duration of diabetes (β = 0.118, p = 0.0047), and presence of diabetes complications (β = 0.197, p = 0.008) were significant predictors of dietary behaviour and accounted for 34.2% of the variance.
Conclusion. Social support, diabetes medications, presence of diabetes complications, and duration of diabetes were associated with improved dietary behaviour. Therefore, social support should be considered when designing dietary interventions for patients with type 2 diabetes mellitus.
Downloads
References
International Diabetes Federation. IDF Diabetes Atlas, 9th ed. Brussels, Belgium: International Diabetes Federation, 2019.
Ministry of Health. Hasil Utama Riset Kesehatan Dasar Jawa Timur 2018. Jakarta; 2019.
Ley SH, Ardisson Korat A V, Sun Q, Tobias DK, Zhang C, Qi L, et al. Contribution of the nurses’ health studies to uncovering risk factors for type 2 diabetes: Diet, lifestyle, biomarkers, and genetics. Am J Public Health. 2016;106(9):1624-30. https://pubmed.ncbi.nlm.nih.gov/27459454. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4981796. https://doi.org/10.2105/AJPH.2016.303314.
Sievenpiper JL, Dworatzek PDN. Food and dietary pattern-based recommendations: An emerging approach to clinical practice guidelines for nutrition therapy in diabetes. Can J diabetes. 2013;37(1):51-7. https://pubmed.ncbi.nlm.nih.gov/24070749. https://doi.org/10.1016/j.jcjd.2012.11.001.
Davies MJ, D’Alessio DA, Fradkin J, et al. Management of hyperglycemia in type 2 diabetes, 2018. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2018;41(12):2669-701. https://pubmed.ncbi.nlm.nih.gov/30291106. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6245208. https://doi.org/10.2337/dci18-0033.
Jannasch F, Kröger J, Schulze MB. Dietary patterns and type 2 diabetes: A systematic literature review and meta-analysis of prospective Studies. J Nutr. 2017;147(6):1174–82. https://pubmed.ncbi.nlm.nih.gov/28424256. https://doi.org/10.3945/jn.116.242552.
Gao J, Wang J, Zheng P, et al. Effects of self-care, self-efficacy, social support on glycemic control in adults with type 2 diabetes. BMC Fam Pract. 2013;14:66. https://pubmed.ncbi.nlm.nih.gov/23705978. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3668988. https://doi.org/10.1186/1471-2296-14-66.
Mohebi S, Parham M, Sharifirad G, Gharlipour Z, Mohammadbeigi A, Rajati F. Relationship between perceived social support and self-care behavior in type 2 diabetics: A cross-sectional study. J Educ Health Promot. 2018;7:48. https://pubmed.ncbi.nlm.nih.gov/29693029. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5903155. https://doi.org/10.4103/jehp.jehp_73_17.
Arda Sürücü H, Büyükkaya Besen D, Erbil EY. Empowerment and social support as predictors of self-care behaviors and glycemic control in individuals with type 2 diabetes. Clin Nurs Res. 2018;27(4):395-413. https://pubmed.ncbi.nlm.nih.gov/28132513. https://doi.org/10.1177/1054773816688940.
Cosansu G, Erdogan S. Influence of psychosocial factors on self-care behaviors and glycemic control in Turkish patients with type 2 diabetes mellitus. J Transcult Nurs. 2014;25(1):51–9. https://pubmed.ncbi.nlm.nih.gov/24084701. https://doi.org/10.1177/1043659613504112.
Kurnia AD, Amatayakul A, Karuncharernpanit S. Predictors of diabetes self-management among type 2 diabetics in Indonesia: Application theory of the health promotion model. Int J Nurs Sci. 2017;4(3):260–5. https://pubmed.ncbi.nlm.nih.gov/31406750. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6626170. https://doi.org10.1016/j.ijnss.2017.06.010.
Gunggu A, Thon CC, Whye Lian C. Predictors of diabetes self-management among type 2 diabetes Patients. J Diabetes Res. 2016;2016:9158943. https://pubmed.ncbi.nlm.nih.gov/27563681. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4987486. https://doi.org/10.1155/2016/9158943.
Primanda Y, Kritpracha C, Thaniwattananon P. Dietary behaviors among patients with type 2 diabetes mellitus in Yogyakarta, Indonesia. Nurse Media J Nursing. 2011;1(2):211-23. https://doi.org/10.14710/nmjn.v1i2.975.
Megananda M. Hubungan antara dukungan sosial dengan kebermaknaan hidup pada pasien diabetes melitus tipe 2. Universitas Islam Indonesia Yogyakarta; 2018. https://dspace.uii.ac.id/handle/123456789/7970.
Misra R, Lager J. Ethnic and gender differences in psychosocial factors, glycemic control, and quality of life among adult type 2 diabetic patients. J Diabetes Complications. 2009;23(1):54–64. https://pubmed.ncbi.nlm.nih.gov/18413181. https://doi.org/10.1016/j.jdiacomp.2007.11.003.
Cradock KA, ÓLaighin G, Finucane FM, et al. Diet behavior change techniques in type 2 diabetes: A systematic review and meta-analysis. Diabetes Care. 2017;40(12):1800–10. https://pubmed.ncbi.nlm.nih.gov/29162585. https://doi.org/10.2337/dc17-0462.
Moore AP, Rivas CA, Harding S, Goff LM. Barriers to following dietary recommendations for type 2 diabetes in patients from UK African and Caribbean communities: A qualitative study. Proc Nutr Soc. 2019;78(OCE1):E31. https://doi.org/10.1017/S0029665119000351.
Kassebaum NJ, Arora M, Barber RM, Brown J, Carter A, Casey DC, et al. Global, regional, and national disability-adjusted life-years (DALYs) for 315 diseases and injuries and healthy life expectancy (HALE), 1990–2015: A systematic analysis for the Global Burden of Disease Study 2015. Lancet. 2016;388(10053):1603–58. https://pubmed.ncbi.nlm.nih.gov/29484919. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6173988. https://doi.org/10.1080/17441692.2018.1444782.
Wallace DD, Gonzalez Rodriguez H, Walker E, , et al. Types and sources of social support among adults living with type 2 diabetes in rural communities in the Dominican Republic. Glob Public Health. 2019;14(1):135–46.
Wu SFV, Huang YC, Lee MC, Wang TJ, Tung HH, Wu MP. Self-efficacy, self-care behavior, anxiety, and depression in Taiwanese with type 2 diabetes: A cross-sectional survey. Nurs Health Sci. 2013;15(2):213–9. https://pubmed.ncbi.nlm.nih.gov/23301516. https://doi.org/10.1111/nhs.12022.
Tang TS, Brown MB, Funnell MM, Anderson RM. Social support, quality of life, and self-care behaviors among African Americans with type 2 diabetes. Diabetes Educ. 2008;34(2):266–76. https://pubmed.ncbi.nlm.nih.gov/18375776. https://doi.org/10.1177/0145721708315680.
Lee YJ, Shin SJ, Wangc RH, Lind KD, Lee YL, Wang YH. Pathways of empowerment perceptions, health literacy, self-efficacy, and self-care behaviors to glycemic control in patients with type 2 diabetes mellitus. Patient Educ Couns. 2016;99(2):287–94. https://doi.org/10.1016/j.pec.2015.08.021.
Published
How to Cite
Issue
Section
License
Copyright (c) 2022 Anggraini Dwi Kurnia, Nur Lailatul Masruroh, Nur Melizza, Yoyok Bekti Prasetyo, Herdianti Nur Hidayani

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
The full license text is available at: http://creativecommons.org/licenses/by-nc/3.0/legalcode.
To request permission to translate, reproduce, download, or use articles or images for commercial reuse or business purposes from the Journal of the ASEAN Federation of Endocrine Societies (JAFES), kindly complete the Permission Request for Use of Copyrighted Material Form and email jafes@asia.com or jafes.editor@gmail.com.
A written agreement will be issued to the requester once permission has been granted.












